Is paracetamol always the best option for antipyretic and analgesic treatment in Dengue?
Dengue is a mosquito-borne viral infection that is widely distributed in tropical and subtropical regions, with a rapidly increasing incidence.
The World Health Organisation (WHO) and the Centres for Disease Control and Prevention (CDC) guidelines recommend avoiding non-steroidal anti-inflammatory drugs (NSAIDs) in suspected or confirmed Dengue infection and advise using paracetamol (acetaminophen) as the preferred antipyretic. Yet, these recommendations are based on physiological reasoning and expert opinion rather than robust clinical trial evidence.
On the other hand, paracetamol may contribute to liver damage in some patients with Dengue.
In this article, we discuss the knowledge gap on the topic.

Contents:
- The hemorrhagic risk in Dengue
- Why is avoiding NSAIDs currently indicated
- Potential harmful effects of paracetamol in Dengue
- Future directions
The hemorrhagic risk in Dengue
While about 70% of Dengue infections are asymptomatic, symptomatic cases carry an intrinsic bleeding risk, from mild to severe.
Mild episodes may manifest as:
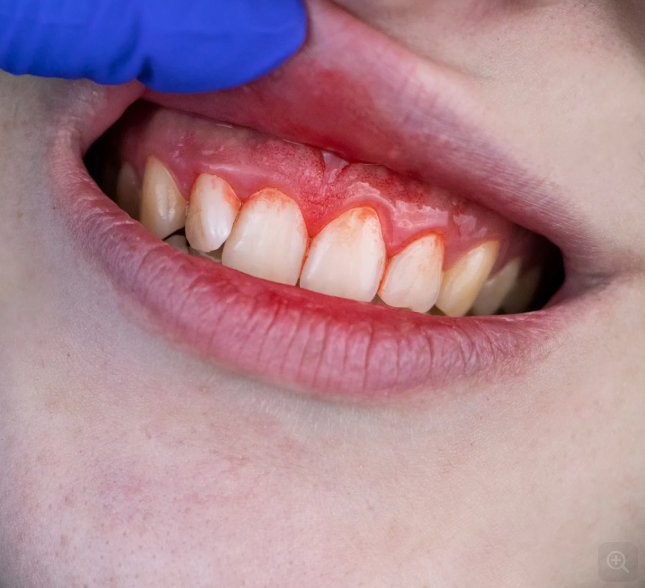
- Minor mucosal haemorrhages such as epistaxis, gingivorrhagia
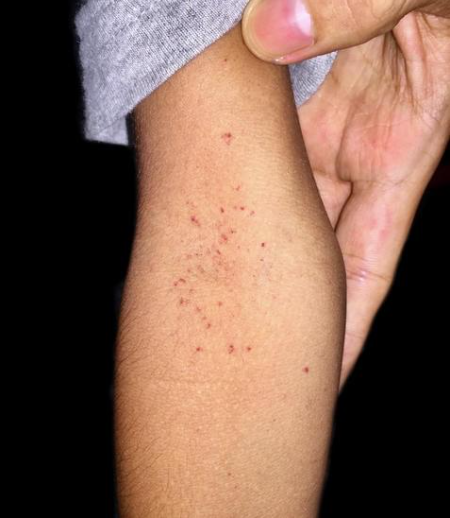
- Minor skin haemorrhages such as ecchymosis, petechiae, and a positive tourniquet test.
Severe episodes may manifest as:
- Haematemesis
- Melena
- Menorrhagia
- Other bleeding manifestations
The pro-haemorrhagic status associated with Dengue infection is a consequence of:
- Thrombocytopenia
- Dengue virus-induced coagulopathy
- Dengue virus-induced vasculopathy
Why is avoiding NSAIDs currently indicated
Non-steroidal anti-inflammatory drugs (NSAIDs) are used globally to treat fever, pain and inflammation. They act by inhibiting cyclo-oxygenase enzyme 2 (COX-2), an enzyme involved in the production of pro-inflammatory mediators.
Non-selective NSAIDs also inhibit COX-1, an enzyme involved in maintaining:
- Gastrointestinal mucosal lining
- Platelet aggregation.
Both COX-1 and COX-2 also play a role in prostaglandin-dependent renal perfusion and glomerular filtration.
For this reason, in Dengue infection, non-selective NSAIDs may contribute to the overall bleeding risk and to gastrointestinal injury. In severe cases of Dengue with hypovolemia and shock, NSAIDs increase the risk of renal damage and acute kidney injury (AKI).
Among all non-selective NSAIDs, aspirin is associated with the highest risk of bleeding due to its irreversible link to COX-1, which causes platelets to be unable to aggregate for the rest of their lifetime. On the other hand, ibuprofen appears to have one of the lowest risks of GI bleeding.
Selective NSAIDs (coxibs), such as celecoxib and etoricoxib, preferentially inhibit COX-2.
For this reason, among all NSAIDs, they are associated with the lowest overall risk of gastrointestinal bleeding. At the same time, they may still contribute to renal toxicity due to prostaglandin-dependent effects on renal perfusion.
Moreover, COX-2 selective inhibitors are associated with an increased cardiovascular risk.
Potential harmful effects of paracetamol in Dengue
Hepatic injury is frequent during Dengue infection and ranges from asymptomatic transaminase elevation to fatal acute liver failure (ALF).
Causes of liver damage during Dengue comprise:
- direct viral effect
- prolonged hypoperfusion
- hypoxia
While paracetamol is generally considered safe at therapeutic doses, it may contribute to liver enzyme elevation in patients with Dengue. In a multicentre randomised controlled trial in adults with Dengue, conducted by Vasikasin et al. and published in The Lancet Global Health in 2019, standard-dose paracetamol was associated with higher transaminase levels compared with placebo, with limited antipyretic and analgesic efficacy.
Future directions
In the absence of safer alternatives, clinicians must balance bleeding risk and hepatic complications when managing fever and pain in Dengue patients.
Until stronger clinical evidence becomes available, current recommendations remain pragmatic rather than evidence-based, highlighting the need for well-designed clinical trials to guide safer symptomatic treatment in Dengue.
Article written by Dr Debora Podestà, Medical Doctor based in Italy, specialised in Infectious Diseases and Hyperbaric and Diving Medicine
Published on December 16, 2025
Review due on December 16, 2028
Sources:
- World Health Organisation: Dengue
- CDC: Clinical care of Dengue
- Vasikasin V, Rojdumrongrattana T, Chuerboonchai W, Siriwiwattana T, Thongtaeparak W, Niyasom S, Lertliewtrakool N, Jitsiri S, Changpradub D. Effect of standard dose paracetamol versus placebo as antipyretic therapy on liver injury in adult dengue infection: a multicentre randomised controlled trial. Lancet Glob Health. 2019 May;7(5):e664-e670. doi: 10.1016/S2214-109X(19)30032-4. PMID: 31000133.
- Kellstein D, Fernandes L. Symptomatic treatment of dengue: should the NSAID contraindication be reconsidered? Postgrad Med. 2019 Mar;131(2):109-116. doi: 10.1080/00325481.2019.1561916. Epub 2019 Jan 16. PMID: 30575425.
- Abdelrahman TG, Gomez-Lumbreras A, Del Fiol G, et al. Nonsteroidal anti-inflammatory drugs and risk of gastrointestinal bleeding: a systematic review and meta-analysis. Clin Pharmacol Ther. 2025. doi:10.1002/cpt.70054